As a homeless father, Dave says taking drugs is the only thing that puts him to sleep.
Under their influence, he’s no longer “bothered about sleeping on the streets” or “worrying about the cold”.
“If I had a nice warm flat, I’d give it up like that,” he says.
The number of people dying from drug misuse in England and Wales is at a record level, while Scotland has the highest rate of drug-related deaths in Europe.
So could drug consumption rooms – where illegal substances are allowed to be taken under supervision – be the answer?
In Sandwell, West Midlands, Dave (not his real name) takes drugs in a disused storage unit at the back of a car park – and calls it “the cage”.
“There’s nowhere else,” he says.
He cleans the area behind the high street and locks the metal gate to prevent children getting inside, mindful of the risk of any used needles being left lying around.
“It just makes me think… what if my daughter trod on one?” he says.
He doesn’t reveal which illegal drugs he takes but says his use spiralled when he became homeless after a break-up.
He no longer sees his daughter or ex-partner.
Dave’s “cage” is one of many areas used as public injection sites across the UK – including underground car parks, stairwells and bin alleys.
Syringes and makeshift tourniquets lie among the fallen leaves, rubbish and debris near a bypass in Sandwell.
“It’s not difficult to understand… why people develop infections and become ill,” says Sue McCutcheon, an advanced nurse practitioner.
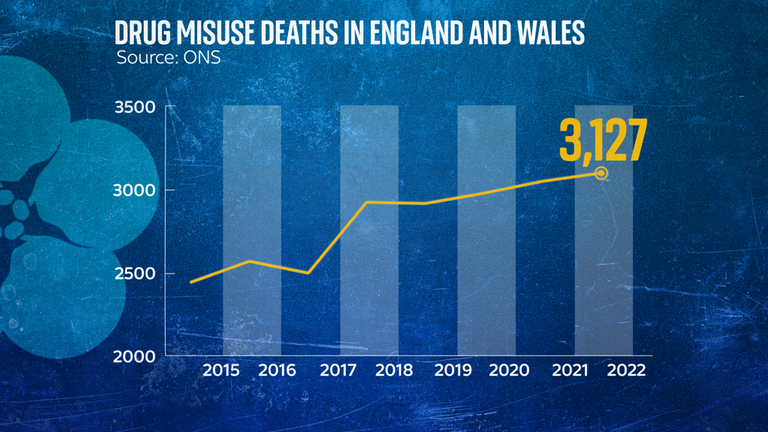
Drug deaths at record high
A total of 3,127 drug misuse deaths were recorded in England and Wales in 2022 – that’s an average of eight people a day.
To put this into context, it’s about the same number of people who died from stomach cancer (3,230 deaths in 2022). But the difference is drug misuse deaths are preventable.
Some 1,051 people in Scotland died from drug misuse in 2022 – its lowest number since 2017 but it remains the highest rate of any country in Europe.
These figures are also underestimates, the Office for National Statistics says, as the specific drugs involved in a death is not always known.
Drug misuse deaths are recorded as those where the underlying cause is drug abuse or drug dependence, or where any of the substances involved are controlled under the Misuse of Drugs Act 1971.
In a bid to reduce the harm around injecting drugs, some countries have introduced overdose prevention centres (OPCs) – also known as drug consumption rooms.
There are around 200 across the world in 17 countries, and Scotland has been given the go-ahead to introduce one this year.
“Most people think inside the drug consumption room it’s fun, everybody’s coming here and doing drugs and high,” says Elisabeth Avril, a GP and director of Espace Gaia, a government-funded centre in Paris.
Most of the 150 people who visit at least once a day are people like Peter Bancelin, who is suffering from withdrawal.
“We often say we come for treatment,” he says.
Before the centre opened, Peter describes “unbearable conditions” with discarded syringes on the floor of public areas and users taking drugs “between cars (with) people passing by to bring their children to school”.
Inside a drug consumption room
Users enter one by one to register, pick up clean equipment and use drugs with a nurse on hand in a room with stainless steel desks, plastic chairs and needle bins.
Staff do not handle the drugs at any point. Users then have access to a “rest room” before they leave.
The centre – which is open seven days a week between 9.30am to 8.30pm – has allowed Peter to do official paperwork, find company and get off the streets.
“Little by little, it’s allowed me to get back on track,” he says.
A study led by Queen’s University Belfast released last month – believed to be the largest evidence review of OPCs worldwide – found they could prevent thousands of deaths and reduce the spread of serious disease.
But the UK government does not support their use and they won’t be allowed in England and Wales over concerns they risk condoning and encouraging the use of illegal drugs.
And not everyone is on board with drug consumption rooms in Paris. There were protests from some residents after the city’s mayor, Anne Hidalgo, signalled she would open four more drug consumption rooms in the French capital.
Read more:
‘I lost my leg to £15 heroin hit’
European capital city may legalise cocaine
Student died after taking ketamine
“Drug policy is not based on evidence – it’s more based on people’s moral preferences,” says Dr Alex Stevens, a criminal justice professor at Kent University, who used to be on the government’s drug advisory committee.
“There’s nobody claiming that an overdose prevention centre is going to solve all the problems we have with drugs.
“But for the people who are most vulnerable to dying, that’s something that can help them continue to stay alive so they can get their lives together.”
In Sandwell, Dave says he would be worried about the police if a drug consumption room was to open near him.
“Where are you going if you’re looking for a shoplifter?” he asks.
Drones deliver overdose treatment
One innovation that has been trialled in the UK with the aim of reducing drug deaths is the use of drones to deliver naloxone, a life-saving medicine which acts quickly to reverse an overdose of opioid drugs such as heroin.
“If somebody is having an overdose, we need to get it to them within at least seven minutes and quicker if possible,” says Dr Paul Royall, a senior lecturer at Kings College London, whose researchers have teamed up with HeroTech8.
When someone calls 999, the call operator activates an emergency response along with the drone, which is expected to beat the ambulance to the scene, allowing the caller to administer the naloxone nasal spray before paramedics arrive.
“So the idea is this reaches the patient first and gives them a bit of extra time so the ambulance can get there and actually really save them,” says Dr Royall.
The team is currently working with drug users in Gosport, on the south coast of Hampshire, before conducting a real-life trial later this year, with a plan to develop the next phase in areas with the most need in the UK.
It estimates delivery costs would be similar to a small Amazon drone delivery – expected to be between £25 and £75 – but says a large-scale roll-out could further bring prices down.
Click to subscribe to the Sky News Daily wherever you get your podcasts
A government spokesperson said: “We are determined to provide those caught in the clutches of addiction with the right support to turn their lives around.
“Our 10-year drug strategy, backed by a record £3bn funding, is tackling both supply and demand for illegal drugs by building a world-class treatment system, alongside relentlessly pursuing and dismantling criminal networks.
“We have already increased the number of people in drug and alcohol treatment by over 17,000, recruited 1,255 drug and alcohol workers and are expanding the availability of life-saving naloxone to prevent more tragic deaths.”